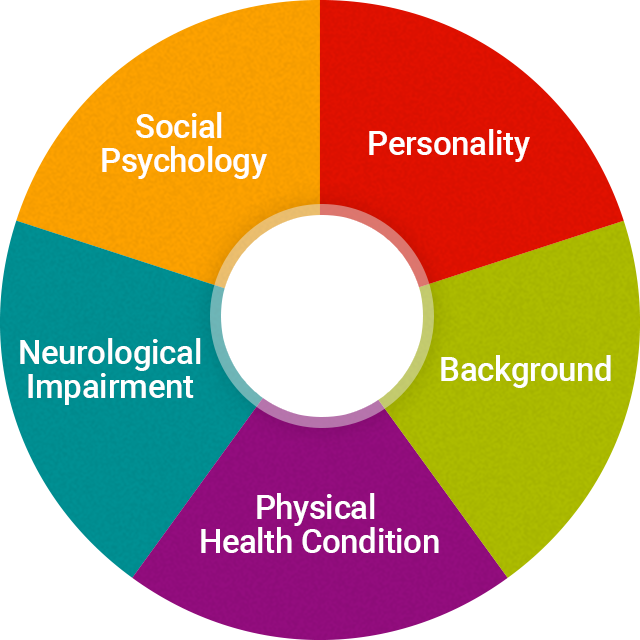
People with dementia in different stages may have changing problems in different areas, such as communication, social skills, mood, and behaviour. They may also have the same behaviour for different reasons. Caregivers thus have to identify the underlying factors that lead to the problems in order to tackle the real issues. This can be done easily with the person-centred care model illustrated below. Please click on the following boxes to learn more.
- Characteristics and interests
Caregivers can arrange activities that match the characteristics and interests of the person. For example, there may be more communication barriers for introverted people to participate in dynamic activities. Caregivers can arrange less dynamic activities like planting, calligraphy and knitting for them. - Lifestyle
The person may have a habit to eat, bath, or work at a certain time of the day. Caregivers can schedule meals, bathing times, and activities according to the habits of the person to increase compliance. - Values and beliefs
Core values and beliefs usually remain unchanged after dementia sets in. Caregivers can utilize those to comfort the person or advise the person to do something. For example, for a person that values family, caregivers can comfort the person by saying, I know you care about us. Just relax.
- Personal history
All the things that happened in the past will affect the beliefs and behaviour of the person. For example, people who worked hard to survive wars may develop a habit of keeping things. Caregivers can tell the person they are putting objects in storage when they are dumping things. - Cultural background
People from different cultures may have different characteristics. For example, Chinese people are concerned more about family, while American people value personal freedom. It is easier for caregivers to accept these characteristics than to change them. - Family and social life
Family traditions may affect the beliefs and behaviour of the person. Friends can also play an important role in shaping our values. For example, it may be better to have sons talk about care plans and living arrangements with very traditional Chinese women to increase their compliance.
- Decline of physical strength
Mobility of the person will continue to decline as dementia progresses. For example, caregivers have to identify whether the person is having difficulty walking or is just too lazy to walk, as the ways to handle each situation are very different. - Adverse effects of medications
Changes in the dosage, type, or brand of medications can have an adverse effect on the person, leading to changes in energy level, mood, and behaviour. Caregivers have to observe the person more closely if there is any change in medications. - Illness and pain
People with dementia may have limited language ability. They may become unresponsive, lose appetite, or become aggressive when they feel uncomfortable. Caregivers thus have to check the physical condition of the person first in case any abnormality is observed.
- Illusions and delusion
Some people may have psychiatric symptoms after they have dementia. For example, they may have illusions such as seeing relatives who have passed away, hearing voices of children playing, and feeling there are bugs on their skin, or delusions such as thoughts of family members trying to fatally poison them or thieves stealing their belongings at night. Caregivers have to watch for the physical condition and emotional responses of the person, be flexible and comfort the person at that moment instead of further provoking the person. For example, caregivers should ask the person if the relatives or children visit very often, and whether they would hurt him or her. This can allow the person to stay connected to the illusion or delusion at that moment while giving caregivers more information. Caregivers should seek advice from a physician as soon as possible afterward. - Emotional control
People with dementia may become more emotional as they encounter more communication barriers due to having fewer cognitive abilities. For example, they may cry when thinking about the past or get angry over tiny issues. Caregivers have to adjust themselves and handle their own emotions to remain calm. - Decline of cognitive function
A person’s cognitive function will continue to decline as dementia progresses, leading to communication barriers and difficulties in self-care. For example, the person may have more and more problems cooking. Caregivers have to assist the person to solve the problem.
- Social needs
Social activities can help people with dementia to maintain cognitive functions and a healthy lifestyle. Caregivers can arrange suitable social activities for the person according to their characteristics, interests and ability. (More details in "Activity Design".) - Family support
People with dementia still have the need for belonging and significance from their family. They also need family members to take care of them. Conflicts with and between family members could be a stress factor for them. - Psychological needs
People with dementia still have the need for purpose, fulfilment and significance. Caregivers should encourage the person to do whatever he or she can, like cleaning up and doing volunteer work. A caregiver can also do a life review for the person to help him or her integrates satisfaction and contentment in life and raises his or her self-esteem.

Problem: The person refuses to eat
Caregivers have tried their best to persuade the person to eat, but the person continues to eat very little. The family members are very worried as the person is losing weight and they can do nothing about it.
Analysis:
Most of us believe that loss of appetite is related to depressed mood. We may as well think that the person with dementia refuses to eat because he or she wants to be fed. However, you can identify many possible reasons with the person-centred care model. For example:
People have different preferences for eating. Some like to eat the same dish every day and some do not; some like to eat with families and some do not. Setting up an environment that is comfortable and matches preferences can increase appetite. Changing the time for meals or having someone else to feed the person may help to reduce suspicion and anxiousness. Caregivers can also introduce the foods and cooking methods or try dishes in front of the person if he or she is feeling insecure.
People have different preferences for eating. Some like to eat the same dish every day and some do not; some like to eat with families and some do not. Setting up an environment that is comfortable and matches preferences can increase appetite. Changing the time for meals or having someone else to feed the person may help to reduce suspicion and anxiousness. Caregivers can also introduce the foods and cooking methods or try dishes in front of the person if he or she is feeling insecure.
Caregivers should look out for the signs of physical illness or pain if the person has no such history. People with dementia may lose the ability to tell their condition as the disease progresses, so the loss of appetite could be the result of stomatitis, uncomfortable dentures, insufficient saliva, physical illness, physical pain, etc. Medical interventions can solve the problem in this case.
People with dementia may lose the ability to recognize some foods as the disease progresses, and they may start to think the seeds in dragon fruit or dark seasonings such as black pepper are bugs. They may also lose the ability to use dining utensils or get confused about what to eat first. If they do not feel hungry, they may stop eating or forget to continue eating instead of seeking help. Caregivers have to provide guidance or support in this case.
While some people may try to seek attention by refusing to eat, some people with dementia may lose appetite because they feel hopeless or helpless and despair of their condition. Some may also think that they are burdens to the family. Caregivers should seek counselling for the person if he or she complains or cries a lot, feels lonely, or is insecure, so that negative thoughts and emotions will no longer decrease his or her appetite.


Problem: Spitting
The person spits despite advice from family members. Caregivers are very frustrated, as scolding cannot stop the person either.
Analysis:
Most of us believe that spitting is a habit the person may have had in the past. Please try to look for other reasons with the person-centred care model. Two possible reasons are included below. Please try to think of another one and replace the “???” in your mind.
Personality
- Little hygienic knowledge
- Habbit
- ???
Background
- Peer influence at young age
- Parents also used to spit
- ???
Physical health condition
- Poor oral hygiene
- ???
- Excessive phlegm
Neurological impairment
- Thinks it is normal
- Obsession
- ???
Social psychology
- Attention seeking
- Complaint
- ???

